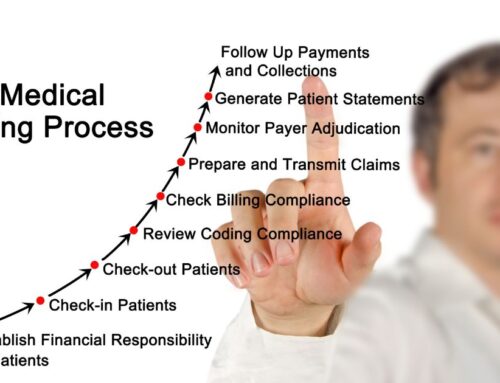
If you’re considering a medical procedure for a patient, you may want to better understand prior authorization in medical billing. Will their insurance cover the procedure you seek? How much will be covered if the procedure is covered? What will their out-of-pocket cost be? These questions often accompany major medical procedures, and the answers could have costly repercussions, both physically and financially, for the patient.
Unfortunately, medical debt in America is significant, with an estimated $88 billion dollars in medical debt showing up on consumer credit records in 2021. Understanding what is and isn’t covered by health insurance, and obtaining prior authorization in medical billing for costly services, can help individuals understand the medical debt they could incur for medical procedures that potentially may not be approved by their plan. Let’s dive into understanding the basics of medical billing and prior authorization in medical billing.
Table of Contents
- What is Prior Authorization in Medical Billing?
- What Role Does Prior Authorization In Medical Billing Play?
- How to Leverage Prior Authorization in Medical Billing
- Credence: A Healthcare Revenue Management Partner who Understands Prior Authorization in Medical Billing
What is Prior Authorization in Medical Billing?
In a medical setting, prior authorization in medical billing essentially means that you or your medical provider billing service have obtained approval from the patient’s insurance provider so that the procedure, prescription, or medical service that they need is covered by the insurance plan you have. By contacting the insurance company, any questions regarding coverage or circumstances in which a procedure would not be covered can be avoided.
Prior authorization in medical billing is typically handled by the medical provider’s office for the individual policyholder, although in some cases a medical group may use a third-party service that will obtain the required pre-authorization on behalf of the medical provider and insured patient.
Without prior authorization, the procedure may not be covered by the insurance plan, which leaves the burden of the cost entirely on the patient. Basically, it’s a clear path to make sure that the insurance provider will approve the medical service and pay for the costs associated with that medically-needed service.
Prior authorization in medical billing is also called preauthorization or precertification; different companies and medical practices use different terminology for essentially the same process of verifying benefits.
What is Considered Medical Services?
Patients may wonder what medical services are considered. Not all procedures that occur in a healthcare-like setting are considered a medical service. For example, an individual who may enjoy the benefits of acupuncture might think it is a medical service when it is not considered an insurable medical service. Fertility treatments, cosmetic procedures, and other elective procedures are often also not considered medical services.
Legally, medical services are provided by a healthcare professional and relate to the diagnosis, prevention, or treatment of any human disease or impairment, or the assessment or care thereof. Healthcare providers must be licensed, registered, and/or certified in accordance with state and federal laws.
When it comes to prior authorization in medical billing, medical services are the billable service provided by the healthcare professional, which could be anything from a prescription drug to a non-emergent yet necessary medical procedure. These services often include treatment for things like cancer or HIV/AIDS, where the procedures, drugs, or treatments are particularly costly or in short supply. Now that we understand what medical services are, let’s take a closer look at the role of prior authorization in medical billing services.
What Role Does Prior Authorization In Medical Billing Play?
When it comes to medical billing, the role of prior authorization may be confusing. Obtaining this preauthorization is confusing to some because they may feel that the insurance policy will either cover medical services or it won’t. However, there are some services that may typically not be covered but that can be covered if prior authorization in medical billing is secured.
From the perspective of the insurance companies, prior authorization is a cost control measure. It helps insurance companies keep their deductibles and premiums affordable because they aren’t paying out for expensive procedures that might not be medically necessary.
From the perspective of medical providers, prior authorization in medical billing can be a frustrating, time-consuming extra hoop to jump through in order to get a patient a medically needed service covered by their insurance.
Prior Authorization Practice Resources
Finding yourself overwhelmed with understanding how prior authorization affects your practice? The good news is that there are a number of resources out there to help medical professionals understand prior authorization in medical billing and the changes that occur as legislation and insurance requirements change.
Those leading medical groups or those in charge of their practice may find that reaching out to a third-party company like Credence Global Solutions who specializes in the complex process of everything from patient experience to medical billing.
How to Leverage Prior Authorization in Medical Billing
Because prior authorization in medical billing is unfortunately an essential process for a medical group or independent medical provider, it is important to consider how to leverage prior authorization to not only prevent patients from being stuck with a hefty bill but to allow the office staff to focus on other more important tasks.
Some medical groups and practitioners opt to handle prior authorization in medical billing internally, however, that can often lead to over-extended staff and wasted resources, errors in obtaining prior authorization, and unhappy patients. You can reduce your administrative burden by using a company to handle things like prior authorization in medical billing.
Keep in mind that if you choose to hire a company, you will want to hire a company that has the time, knowledge, and resources to secure prior authorization in medical billing for your practice and your patients, you can save thousands as there are fewer errors, reduced operational costs, and enhanced compliance and revenue, all with the security and compliance that your practice needs.
Where to Find Medical Billing Services in Dallas
Outsourcing services like prior authorization in medical billing is a huge consideration for medical groups and practices all over the country, especially medical practices looking for medical billing services in Dallas. Some have concerns about there being issues with time zones, language barriers or misunderstanding regarding state or federal regulations with foreign companies outside the U.S., and overall ease-of-use being a problem.
Fortunately for those located in Texas, you can find leading a medical billing company in Dallas. Credence has multiple convenient locations across the United States and has its company headquarters located in Dallas. Your practice will appreciate the benefits of a local third-party service like Credence Global Solutions for prior authorization in medical billing in Dallas.

Credence: A Healthcare Revenue Management Partner who Understands Prior Authorization in Medical Billing
Are you ready to utilize a service that offers prior authorization in medical billing? Credence is here to help. We are a healthcare revenue management partner who not only understands prior authorization in medical billing but we also understand the high demands on your practice from both insurance providers and your patients.
When you choose to work with us, you can be confident in knowing that you are using a company well-equipped to handle your practice or medical group’s volume of services and that will effectively handle your patient’s prior authorization in medical billing needs.
Speak with one of our medical billing services experts to learn more about how we can help with prior authorization in medical billing.